Flashes and Floaters
Background
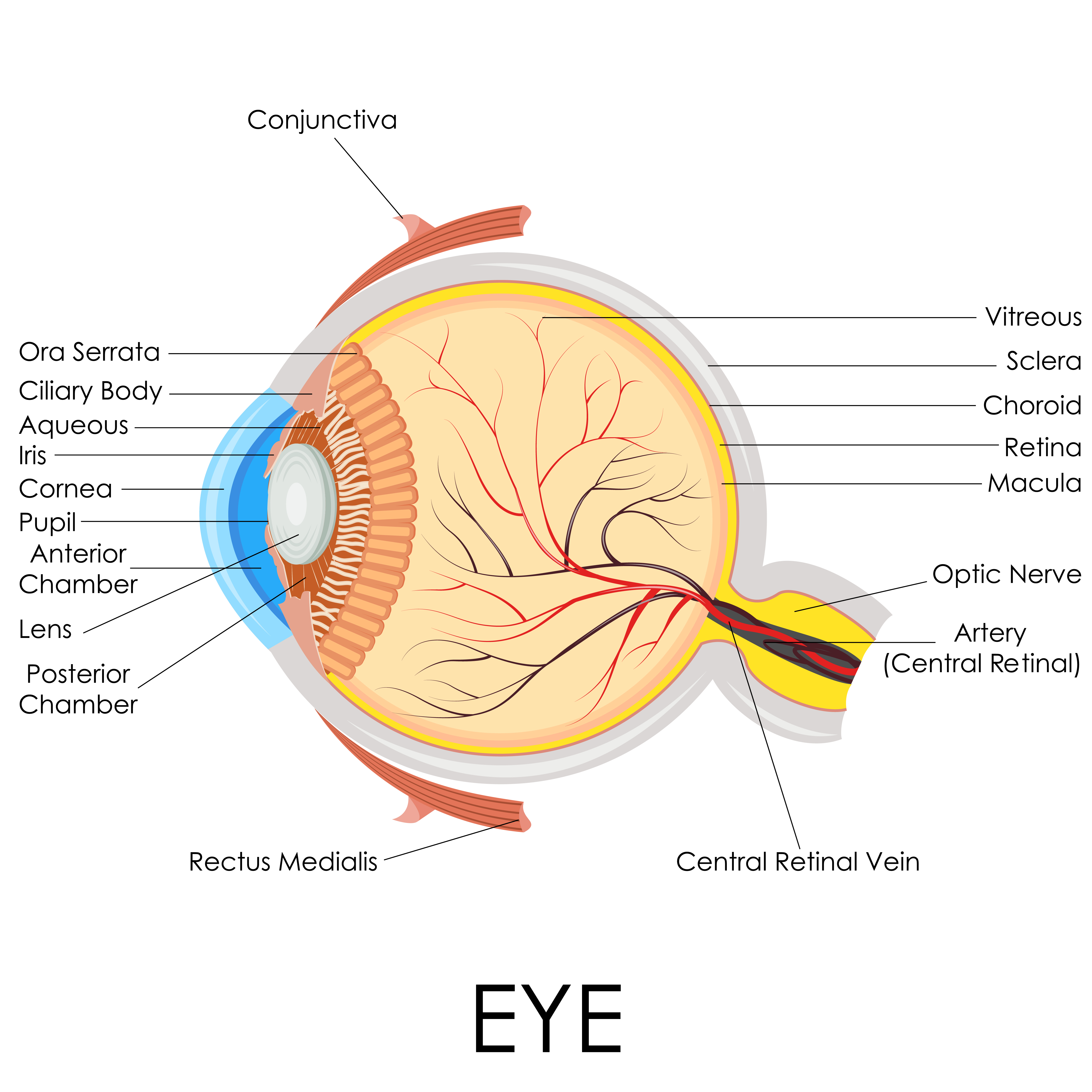
Figure 1
For most individuals the separation of the vitreous gel from the retina brings no significant consequences. A small proportion of patients will, however, develop problems from this naturally occurring process. This can range from having a small bleed within the eye, which may settle with time, to having a retinal tear which will need treatment, or potentially even a retinal detachment (Figure 2) which will require surgery. Only an examination by an ophthalmologist will determine the extent of treatment required.
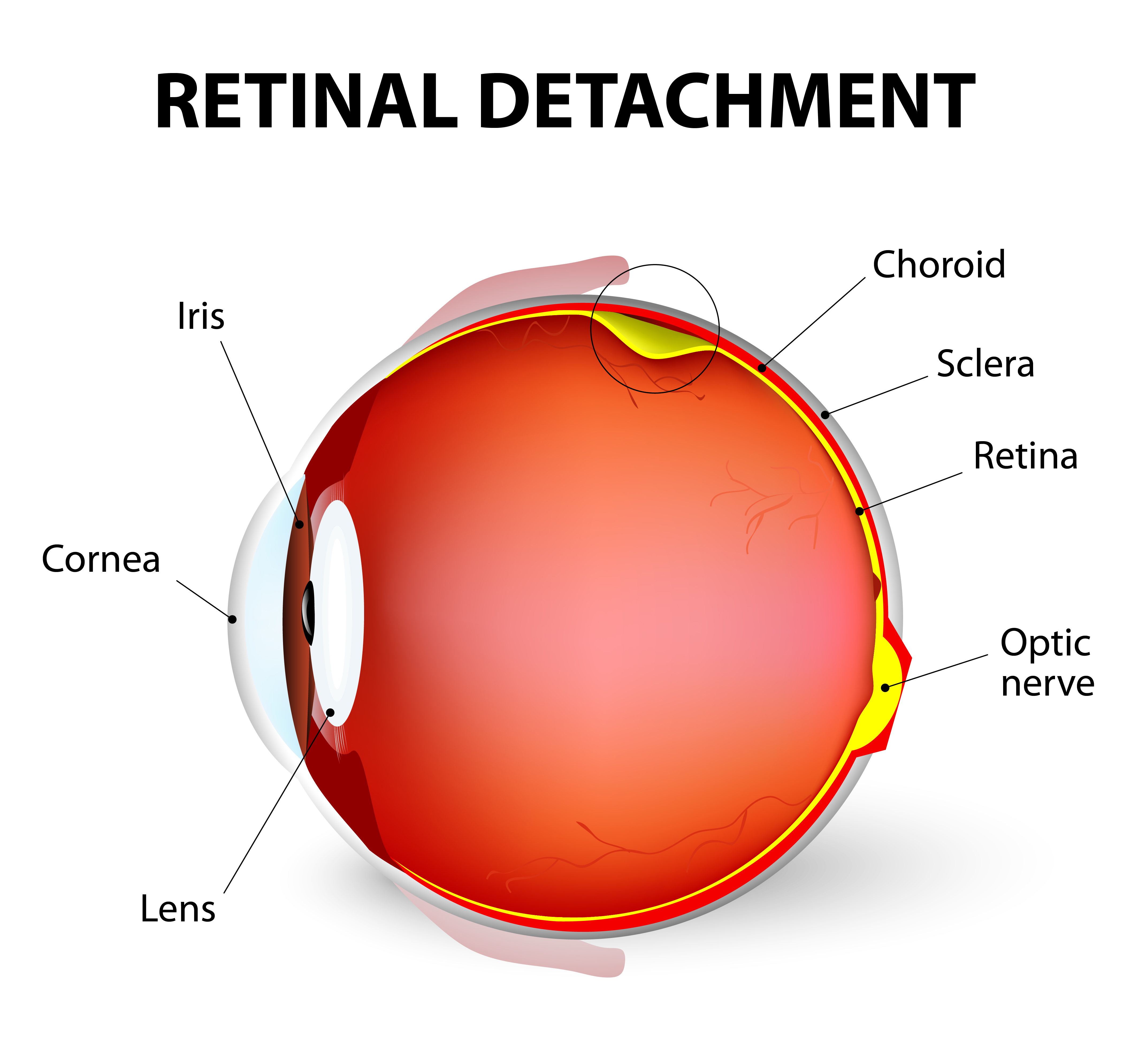
Figure 2
Symptoms
Treatment Options
- Significant increase, or burst of new floaters
- Significant increase in flashing lights, or persistence of flashing lights
- A dark shadow developing in the visual field which is fixed and immovable
If after a thorough examination a retinal tear is detected, then usually your ophthalmologist will suggest that you should have a laser treatment to the area around the retinal tear, to stop this progressing to a retinal detachment. This would be done under local anaesthetic and the aim is to prevent this small tear in the retina progressing to something more serious such as a retinal detachment (Figure 2).
If a retinal detachment is observed following your examination, this will need treatment by a vitreo retinal specialist and the outcome will depend upon the extent of the retinal detachment at examination.