Glaucoma
What is glaucoma?
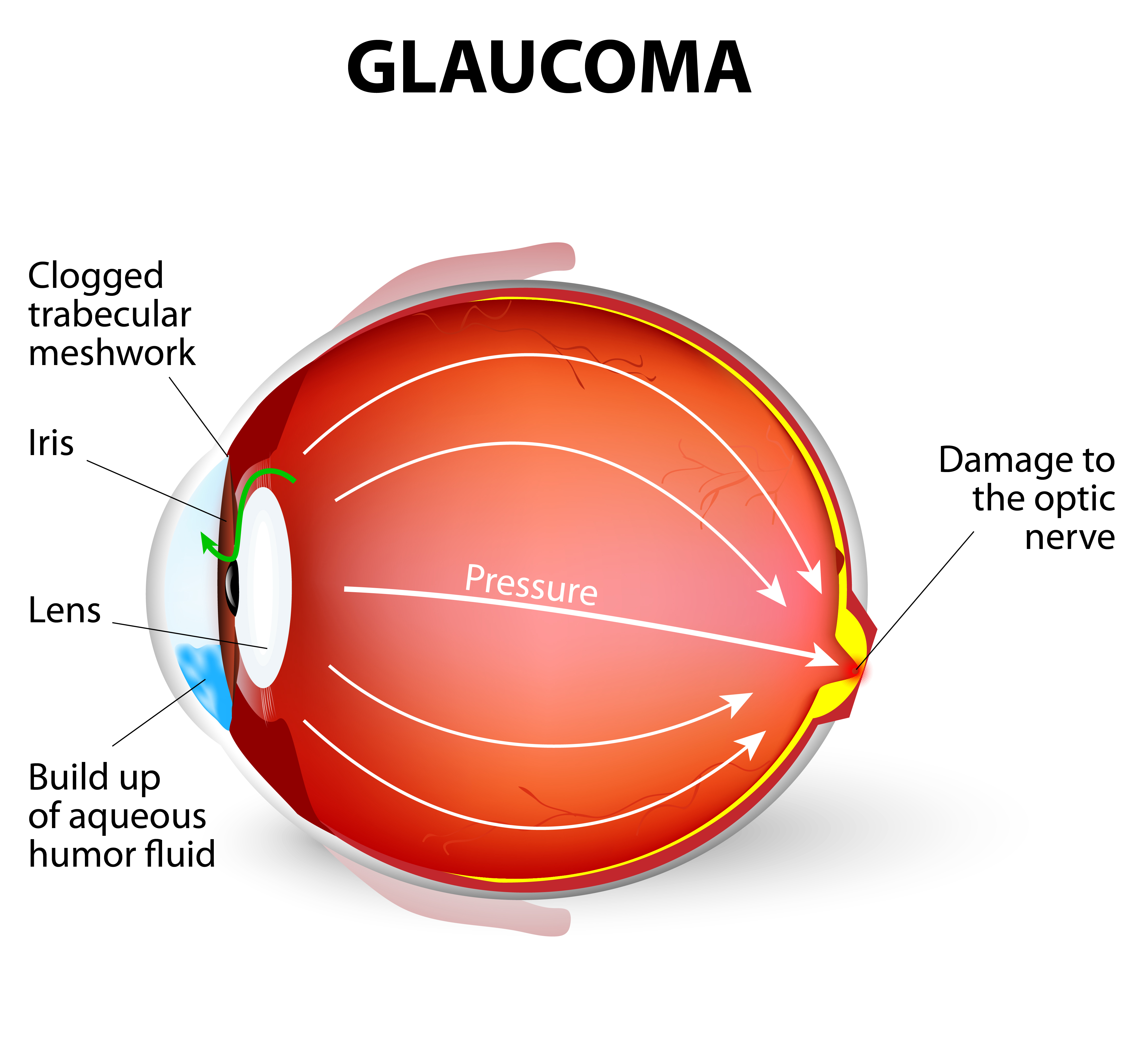
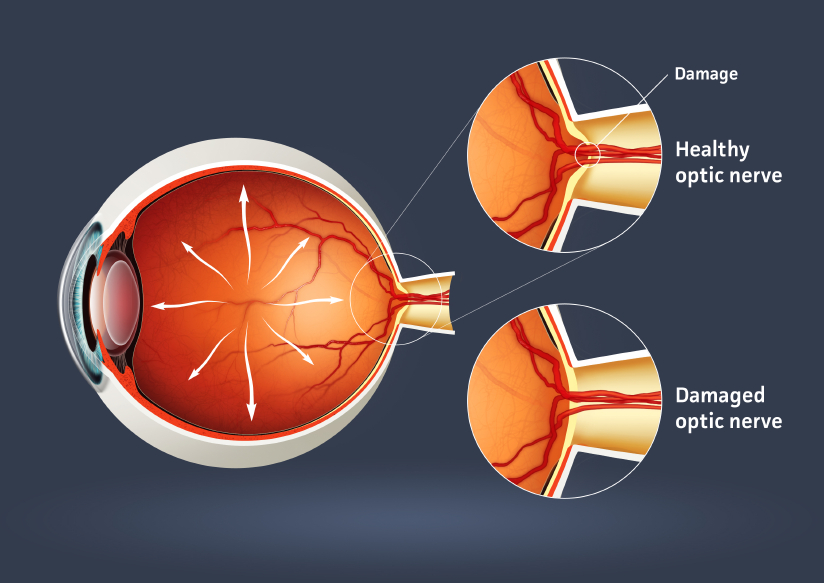
Figure 2.0 mechanics of damage to the nerve in glaucoma
How does it affect me?
Glaucoma is typically diagnosed through the recognition of raised intraocular pressures (IOP) during an eye examination. This may sometimes prompt further investigation such as visual field testing, or alternatively optical coherence tomography (OCT) testing of the optic nerve, which may demonstrate evidence of glaucoma.
If glaucoma remains untreated for a long time, then the patient may then start to notice the peripheral vision being less sensitive. If at this point the condition is not treated, then visual field may continue to become restricted which will eventually lead to significant visual loss. Glaucoma rarely leads to total loss of sight, but can cause significant symptoms secondary to loss of peripheral vision.
Why do people get glaucoma?
How is it treated?
Additionally more objective measurements such as optical coherent tomography (OCT) or Heidelberg Retina Tomography (HRT) of the optic nerve head will be undertaken, to allow us to determine to amount of damage that has occurred at the optic nerve (Figure 3.0 and 4.0) At the first visit, often many measurements will be taken as a baseline, in order to allow more effective management in the future.
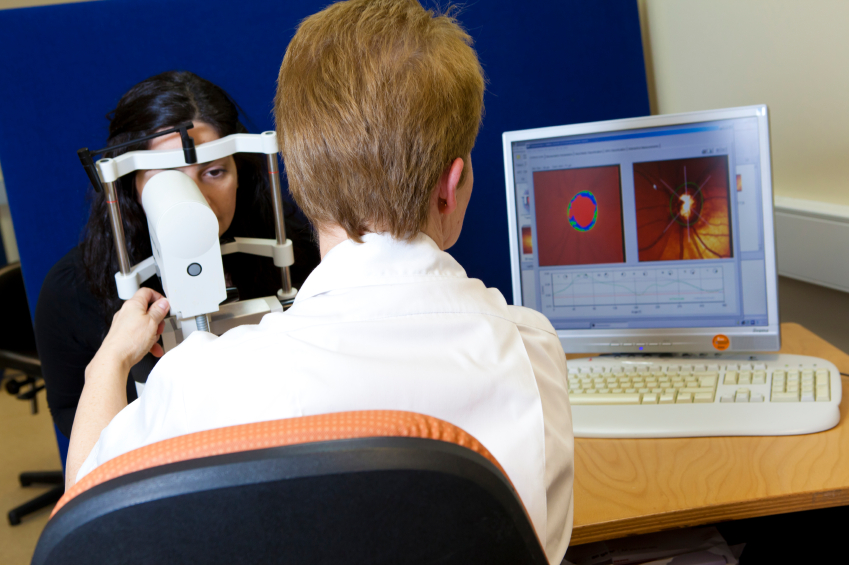
Figure 3 HRT imaging of the optic nerve
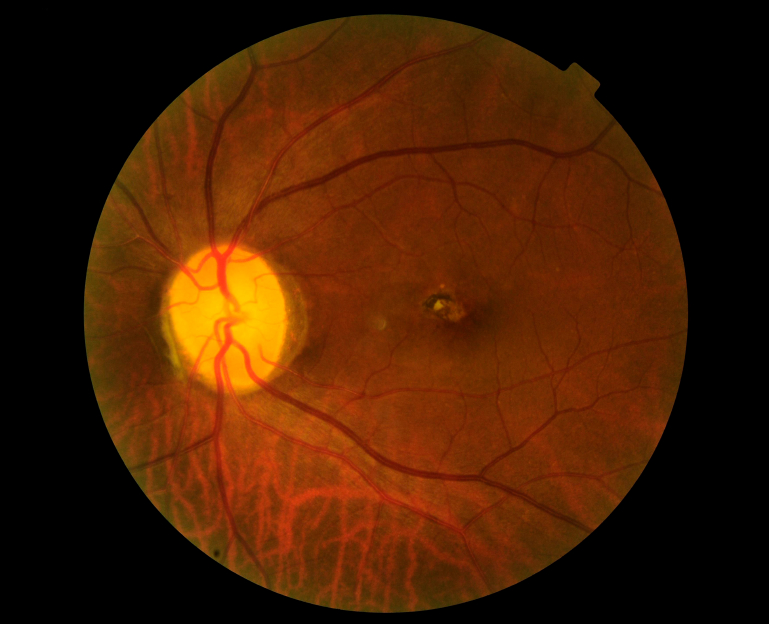
Figure 4 shows a pale disc which results from glaucoma
If it becomes apparent that the prescribed drops are not lowering the pressure to an adequate degree, then there are further drops which can be added.
Sometimes it may not be possible to control the intraocular pressures to a satisfactory degree with drops alone, in which case laser can sometimes be used, or even surgery. Typically surgery is reserved for when glaucoma is difficult to manage.